CCTG CLC.2/Alliance A041202 demonstrated superior progression-free survival at 2 years with ibrutinib alone (87%; HR 0.39) or ibrutinib-rituximab (IR 88%; HR 0.38) compared to chemo-immunotherapy with bendamustine-rituximab (BR 74%) in treatment-naïve patients (pts) with chronic lymphocytic leukemia (CLL) who were 65 or older (Woyach NEJM 2018). We hypothesized that ibrutinib-based therapies would be more costly than BR but that costs would be offset by less toxicity and improved quality of life (QOL). We completed a prospective trial-based economic analysis to study the direct medical costs and quality-adjusted benefit associated with ibrutinib-based therapies compared to BR in the Canadian (CDN) subset of patients enrolled in CLC.2/Alliance 041202.
All CDN pts were invited to participate in the companion analysis. Health utilities were collected using the EuroQOL EQ-5D and calculated using CDN population valuations (Bansback PLOS One 2012). Resource utilization forms were administered to collect off-protocol health care encounters. The planned analysis was a cost-utility analysis from the perspective of a public healthcare system, examining the costs and outcomes (quality-adjusted life years or QALYs) of ibrutinib-based therapy compared to BR. Unit costs were applied to resource data based on publicly available provincial/national databases; all costs were expressed in 2019 US dollars (1 CDN = 0.75 US dollar). Total and disaggregated direct medical costs are presented descriptively. Mean survival was calculated using the restricted mean survival method from randomization to the study time-horizon of 24 months; derived utilities were used to calculate QALYs. A discount rate for costs and benefits (r=0.05) was applied. The analysis was based on estimation (with bootstrapping) of an incremental cost-effectiveness ratio (ICER) and/or direct medical costs.
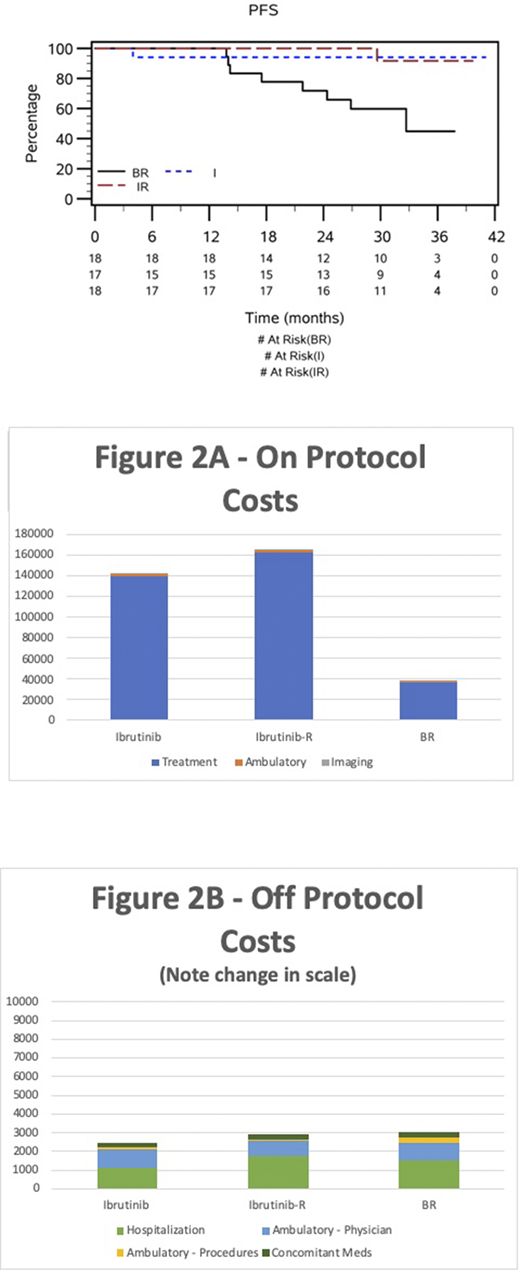
A total of 55 pts were enrolled; two pts who did not receive any treatment were censored at day 1 and 3 after randomization and excluded from analysis. Of the 53 analysed, pt demographics were well balanced between treatments and were reflective of the entire population: mean age was 71.6 (SD 6.34) in pts receiving ibrutinib alone (n=17), 72.2 (SD 3.85) in pts receiving IR (n=18), and 71.7 (SD 4.1) in pts receiving BR (n=18). A total of 3 pts, one in each arm, had 17p deletion. Progression-free survival at 2 years for CDN pts was 94% (95% CI 65-99%) for ibrutinib, 100% (95% CI 100-100%) for IR, and 72% (95% CI 45-87%) for BR (Figure 1). At 24 months, 1 pt on the BR arm had crossed over to ibrutinib (as per protocol); there was no overall survival difference between the three arms. On-protocol costs (including protocol treatment, ambulatory care, and imaging) and off-protocol costs (including hospitalizations, concomitant medications, and ambulatory care) are highlighted in Figure 2. On-protocol costs were higher for pts receiving ibrutinib (mean $142,001 USD; SD 48,417) and IR ($164,931; SD 46,208) compared to BR ($38,509; SD 10,351), driven by higher drug acquisition costs associated with ibrutinib (list price $6422 for 420mg/30 days). In contrast, off-protocol costs were modestly higher for pts on BR (mean $3050; SD 3812) compared to the ibrutinib ($2460; SD 3863) or IR ($2890; SD 4206); hospitalizations were the key off-protocol cost drivers and were highest for pts on IR and BR. Overall mean costs over the 2-year time horizon were $144,461 (SD 47,910) for pts on ibrutinib, $167,820 (SD 46,830) for pts on IR, and $41,560 (SD 11,849) for pts on BR. Discounted QALYs were similar between the three treatment arms: 1.66 (0.16) for ibrutinib alone, 1.65 (0.24) for IR, and 1.66 (0.17) for BR. Given the similar quality-adjusted survival between arms at the time of this analysis, a formal ICER was not calculated.
Direct medical costs are substantially higher for pts receiving continuous ibrutinib-based therapies, compared to chemo-immunotherapy of fixed duration, in frontline CLL management; the key cost driver is the cost of ibrutinib. The PFS benefit with ibrutinib-based therapy has not translated into an advantage in quality-adjusted survival to date; further follow-up may be required to demonstrate any cost or QOL benefits associated with fewer progression events for those on ibrutinib.
Support: U10CA180821, U10CA180882; U10CA180863 and #704970 CCTG. https://acknowledgments.alliancefound.org ClinicalTrials.gov: NCT01886872
Owen:AbbVie, F. Hoffmann-La Roche, Janssen, Astrazeneca, Merck, Servier, Novartis, Teva: Honoraria. Lam:Roche: Honoraria, Speakers Bureau; Janssen: Honoraria, Speakers Bureau. Crump:Servier: Consultancy; Kite/Gilead: Consultancy; Roche: Consultancy. Sperlich:Lundbeck Canada: Honoraria. Woyach:Pharmacyclics, Janssen, Morphosys, Karyopharm, Verastem, Abbvie, Lox: Research Funding; Janssen, Pharmacyclics, AstraZeneca, Abbvie, Arqule: Consultancy; Pharmacyclics LLC, an AbbVie Company, AbbVie, Janssen, AstraZeneca, ArQule: Honoraria. Prica:astra zeneca: Honoraria; seattle genetics: Honoraria; Gilead: Honoraria. Hay:Roche: Research Funding; Janssen: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal